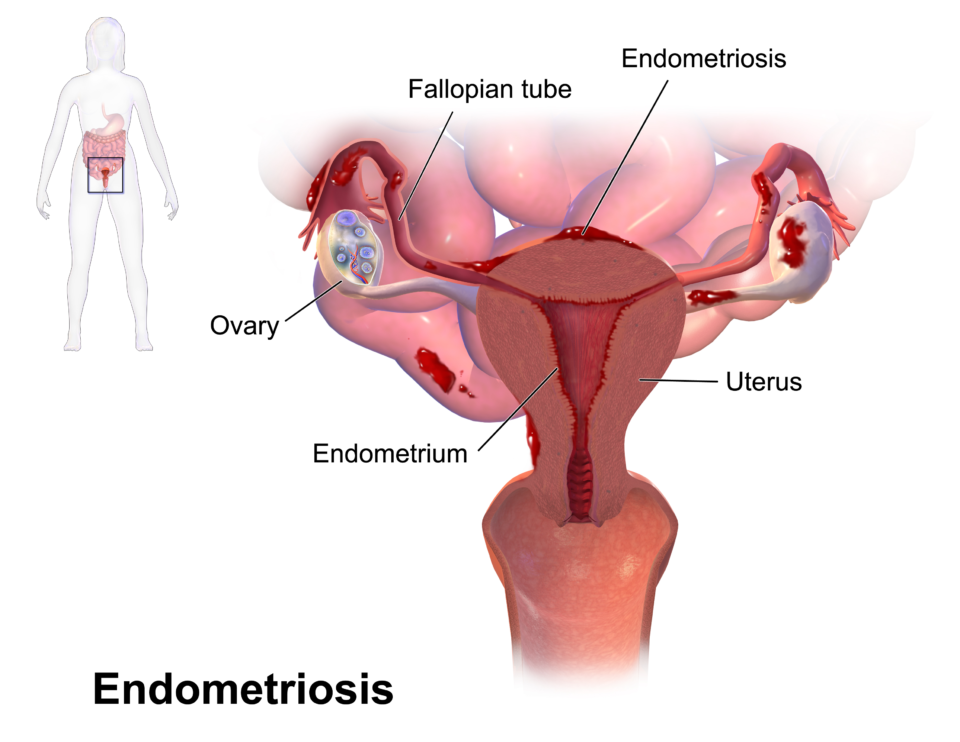
Endometriosis is a chronic gynecological condition where tissue similar to the uterine lining grows outside the uterus, often leading to persistent pelvic pain, painful periods, and reduced quality of life. While there is no universal cure, modern medicine offers a range of effective pain management strategies tailored to symptom severity, age, and reproductive goals.
This article focuses on medical (non-surgical) approaches used to control pain and improve daily functioning.
Understanding Pain in Endometriosis
Pain associated with endometriosis is complex and multifactorial. It may result from:
-
Inflammation triggered by misplaced tissue
-
Hormonal stimulation of lesions during the menstrual cycle
-
Nerve irritation or sensitization
-
Muscle spasms in the pelvic floor
Because pain mechanisms vary between individuals, treatment often requires a personalized and stepwise approach.
First-Line Medical Treatments for Pain Relief
Nonsteroidal Anti-Inflammatory Drugs (NSAIDs)
NSAIDs are frequently the initial treatment choice for mild to moderate pain.
How they help:
-
Reduce inflammation
-
Block prostaglandins responsible for menstrual pain
Common options include:
-
Ibuprofen
-
Naproxen
Limitations: NSAIDs may be less effective for severe or chronic pain and can cause gastrointestinal side effects with long-term use.
Hormonal Therapy: The Foundation of Medical Management
Hormonal treatments aim to suppress ovulation and menstruation, reducing lesion activity and inflammation.
Combined Oral Contraceptives (COCs)
These are widely prescribed due to their effectiveness and accessibility.
Benefits:
-
Regulate or stop periods
-
Reduce menstrual and pelvic pain
-
Can be used continuously for better symptom control
Progestin-Based Therapies
Progestins counter estrogen’s effects on endometrial tissue.
Common forms:
-
Oral progestins
-
Injectable formulations
-
Hormonal intrauterine devices (IUDs)
Advantages:
-
Decrease lesion growth
-
Lower pain intensity
-
Suitable for long-term use in many patients
Advanced Hormonal Treatments for Moderate to Severe Pain
Gonadotropin-Releasing Hormone (GnRH) Agonists and Antagonists
These medications create a temporary low-estrogen state, similar to menopause.
Pain relief mechanisms:
-
Suppress ovarian hormone production
-
Reduce inflammation and lesion activity
Important considerations:
-
Often combined with “add-back therapy” to reduce side effects
-
Typically used for limited durations due to bone density concerns
Aromatase Inhibitors
Used in selected cases where other therapies fail.
Key features:
-
Reduce estrogen production at tissue level
-
Often combined with other hormonal agents
-
Reserved for refractory pain cases
Adjunct Medical Therapies for Comprehensive Pain Control
Neuropathic Pain Medications
When nerve involvement is suspected, certain medications can help modulate pain signals.
Examples include:
-
Gabapentinoids
-
Low-dose antidepressants used for pain modulation
Pelvic Floor Muscle Relaxants
These may be prescribed when muscle tension contributes to pain, particularly during intercourse or bowel movements.
Individualizing Treatment Plans
Successful pain management depends on multiple factors:
-
Severity and pattern of pain
-
Response to previous treatments
-
Desire for fertility
-
Tolerance to side effects
A stepwise strategy allows adjustments over time, ensuring both symptom relief and long-term safety.
Monitoring and Long-Term Management
Endometriosis is often a lifelong condition, making ongoing follow-up essential.
Regular evaluation helps:
-
Assess treatment effectiveness
-
Modify therapy as symptoms change
-
Minimize medication-related risks
Frequently Asked Questions (FAQs)
1. Can medical treatments completely cure endometriosis pain?
Medical treatments manage symptoms effectively but do not eliminate the disease entirely. Pain may return if therapy is stopped.
2. How long does it take for hormonal treatments to reduce pain?
Many patients notice improvement within 1–3 months, though full benefits may take longer.
3. Are hormonal treatments safe for long-term use?
Some options are suitable for extended use under medical supervision, while others require time limits and monitoring.
4. What happens if pain does not improve with medication?
Persistent pain may require treatment reassessment, combination therapy, or consideration of non-medical approaches.
5. Can teenagers with endometriosis use these treatments?
Yes, many hormonal and non-hormonal therapies are appropriate for adolescents when prescribed carefully.
6. Do these treatments affect future fertility?
Most medical treatments are reversible and do not permanently impact fertility.
7. Is it normal to need multiple treatments over time?
Yes, endometriosis pain often evolves, and treatment plans may change as symptoms and life circumstances shift.